On April 2, I received a heart-dropping text: “Rich Pickett was put on a ventilator due to COVID. Praying for our friend.”
It was the first that I heard that he was sick. And COVID-19? A ventilator? The sinking feeling deepened. The reality of the virus flooding media outlets suddenly hit home with a punch.
As you may know, Rich is a regular Twin & Turbine contributor and very involved, passionate pilot. He is also a good friend. It was impossible to imagine anything dampening his incredible energy. (Seriously, I can barely keep up with him at tradeshows!).
Over the next week and a half, I joined countless others in prayers for Rich and his family and followed the daily Facebook updates on his progress.
To our extreme joy, on April 11, he awoke! The day before Easter. He has since baffled everyone with the rapid rate of his recovery. Just two weeks after leaving the hospital, he was back in the air. And now he has returned to an active schedule of working, flying, traveling, biking, etc. Simply amazing.
But, I will let Rich take it from here. Below he shares a recount of the experience, along with his current mission to assist the healthcare community and recognize the medical staff who saved his life.
Welcome back, Rich. Twin & Turbine and the general aviation community are so fortunate to have you.
COVID – A Pilot’s Experience
by Rich Pickett
“Will I pass my First Class flight physical?”
This was one of my first thoughts when I awakened from an induced coma due to COVID-19. I was in the Intensive Care Unit at Kaiser Permanente San Diego Medical Center. While I was surprised to be alive, keeping our medical certificate is critical as pilots!
Twelve days earlier, I had entered the Emergency Room at Kaiser. In an act of stubbornness, I did not go to the hospital until my COVID test could be confirmed, which was not advantageous. I had been at home with a high fever and building pneumonia for over a week prior. Using a pulse oximeter my blood oxygen saturation, which is usually 99, was in the 80s resting and lower when standing – not a good sign. It was time to go to the hospital.
Arriving at the ER, my wife Jane was told to stay in the car. I was helped out and into a wheelchair. It was April 1 – April Fools’ Day. I waved goodbye. That would be the last time I would be with her for 17 days.
In the ER, I texted my family financial account details, transferred cash to make sure they wouldn’t have to worry, and told Jane that I hoped she didn’t become infected. I texted one of my friends to sell our SR22 and Eclipse if I didn’t survive, then basically said goodbye to my family. I turned off my phone so I wouldn’t see their replies. At that time, I didn’t expect to survive the night. I later learned that my family shared the same thoughts regarding my survival.
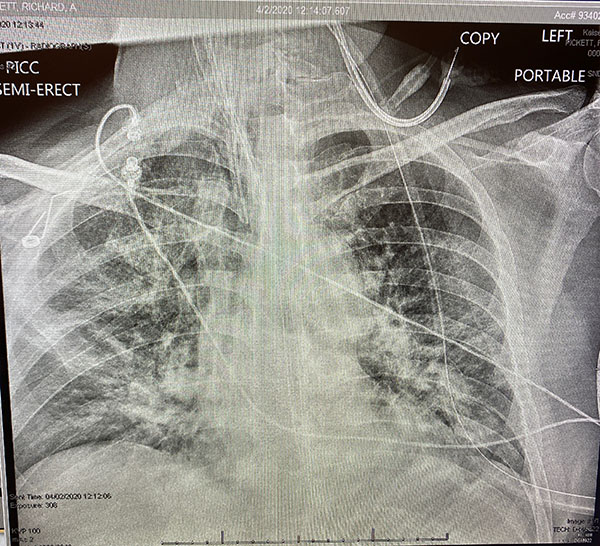
Sherri Case, the ER nurse who first helped me, made me comfortable after the X-ray of my lungs. (It looked like someone had stuffed them with cotton candy!). I signed permission forms for ventilation as well as a “Do Not
Resuscitate” authorization in case the ventilation didn’t work. I thought to myself, “I have had an amazing life, wonderful family and friends, flown extensively, helped a number of people, and this was just another phase.” I then basically passed out, waking up 11 days later in the ICU.
Dr. Vi Bowman, an infectious disease expert at Kaiser, and experienced with Ebola, SARS and other diseases, was one of my medical team. Dr. Bowman approached Jane and asked if she thought I would want to be involved in a drug trial with Remdesivir. Jane, who has a Ph.D. in Biopsychology and Neuroscience, knew I would want to consent, no matter the outcome. At that time, little was known about Remdesivir, however, it looked promising. And since I was considered a very severe case, it was worth a try. I became a clinical trial test subject.
Awake!
Awaking with the ventilator apparatus inserted through my larynx, I could only use rudimentary sign language to communicate. Simon and Anna, two of my many wonderful nurses, tried hard to understand my version of charades. With my arms restrained to keep me from pulling out the tubes, I motioned that I wanted it removed. It wasn’t particularly painful, just uncomfortable. It felt as if I was choking when coughing. I was ready to progress to the next phase – surviving. Apparently, I was very convincing as Dr. Tauseef Siddiqi, one of my ICU pulmonologists, along with Dr. Vigi Sankar and Dr. Randy Dalugdugan, agreed to remove it two days earlier than planned.
I wondered when they would remove the tube when suddenly I saw one of the nurses in front of me say, “1, 2, 3, pull!” That question was quickly answered. With the ventilator removed, the day before Easter, I still had a significant case of double pneumonia and fever to overcome, so another course of intravenous antibiotic was ordered.
Now breathing on my own, which was very painful with the pneumonia and coughing, my next step was to recover. I thought, “Here I go again.” If I didn’t fight hard enough and prove I could do it, they would intubate me again. At this point, I had lost more than 25 pounds during the first 12 days, which resulted in significant weakness. Still on phenobarbital, and with some of the sedatives still in my system, it was like flying through clouds without instruments – difficult to understand exactly what I was doing. Even under these conditions it was important to build my strength, so I started my own exercise program that day. At first, I could only raise my legs an inch or two, and simply lifting my arms was almost impossible. I looked at my legs and the muscles appeared to have disappeared. So much for mountain biking with Jane.
When I came out of the induced coma, my vision was in bad shape. Again, my first thought was my medical. I couldn’t open up my left eyelid fully, and when I could, the vision in that eye was very poor and my depth perception was impacted. Ana knew I was a pilot and would repeatedly tell me to open my eyes. I then resigned to myself that if it didn’t improve, Jane needed to complete her BFR so we could fly. Over the next several days I worked to focus my vision by doing my own eye exercises and using anything I could find as an eye chart. Within four days, my vision was almost normal – one less concern for my medical.
Two days later, I was out of the ICU, and still in isolation, moved to another floor. I told the nurses to avoid coming into my room unless necessary since I knew they could be exposed to the virus and the last thing I wanted was for them to get ill as well. The care and concern of the medical staff was simply amazing, and I immediately made it my primary goal to remember as many names as possible to thank them later. I would tell my doctors to just call me on the phone, however, they insisted on visiting in person. Every day housekeepers, orderlies, therapists, nurses would don multiple layers of protection to care for me. My sister Diana and my son Tigre started a fundraiser to purchase PPE for the Kaiser staff and other hospitals.
Three days after the ventilator was removed, I told one of my physicians that I would be leaving the hospital in three more days. Dr. Sapna Iyer politely told me it was her decision, not mine. I thought to myself I need to prove to her it could be done, and it became another goal!
The next day, a good friend of mine, a cardiologist and a pilot, told me he wanted to do a flyby of the hospital. He texted me from the Montgomery Airport (KMYF) that he was about to depart, knew where my room was located, and that it faced the base leg to Runway 28R. A few minutes later, Paul Teirstein, flies by my window in his Great Lakes and wags his wings. It was truly a wonderful sight.
The following day, two days after I told Dr. Iyer I would be leaving in three, she came into my room and said to me, “You are medically cleared. You need to write a story!” During my stay in the ICU, and afterward, a number of my friends contacted the staff directly and told them about my passion for flying, volunteer work and Angel Flight West. They knew I wanted to get back to flying as soon as possible.
I also learned that Jane had contracted the coronavirus from me, but thankfully she had relatively mild symptoms. I was relieved to hear that, and it also meant I wouldn’t have to quarantine away from her. Discharged, with no prescribed medications, I wheeled out of the hospital into her arms!
Recovery
Recovery wasn’t easy. During my two weeks of quarantine, I struggled each day to walk a few more steps, do more work around the house, work longer hours on my aviation business, continue my projects as the Safety Officer of Angel Flight West, and talk with the large number of friends who reached out with prayers and kind thoughts. I used a walker for two days, moved to a cane for three more, then put them away. I was determined to work as hard at recovery as the doctors and nurses did to save my life.
On the last day of my quarantine, Jane and I took to the skies in our Cirrus SR22. It was tough moving the heavy doors to our hangar, but it felt so good. We went up and did an entire series of steep turns (one of our favorites), toured the San Diego countryside and practiced an approach. The next day a friend of ours, Mike Turk, joined me in our Eclipse, both of us with masks, to make sure that I could fly that as well. I was teaching one of my Eclipse clients two days later and completed my Eclipse recurrent the following day with a PPE.
Ten days after my quarantine, I was off to FlightSafety at DFW for my PC-12 recurrent, flying my Eclipse to Texas. It was surreal to be at one of the largest airports in the world and experience the lack of traffic. I love airplane noise, so I missed that. I resumed my Part 135 charter flights the day after returning from FlightSafety.
Before every flight, I assess whether or not I am safe to fly, except now with more diligence. My AME and friend, Dr. John Raniolo in Phoenix, Arizona, was in contact with me during my recovery to ensure I was medically ready to fly. One month after my quarantine ended, he renewed my First Class Medical Certificate.
I remembered the pledge to myself to recognize the medical staff and others at Kaiser. I wrote a long detailed letter to the Kaiser Board of Directors, identifying as many people as I could remember, describing the passion and care of their colleagues. I probably didn’t realize the true impact of my experience upon my family, friends and the staff at Kaiser until I wrote that letter and it was published widely in our community. One nurse told me afterward that she had been anxious about going to work due to the virus. After she read my letter thanking the staff and the difference she made in my life, she felt she could conquer the world!
Like those who help all of us on a daily basis, it is important to remember how others are impacted by diseases such as SARS-COV-2. Be safe, and enjoy the wonderful opportunity we have to fly above this unique planet.








